November 9, 2018
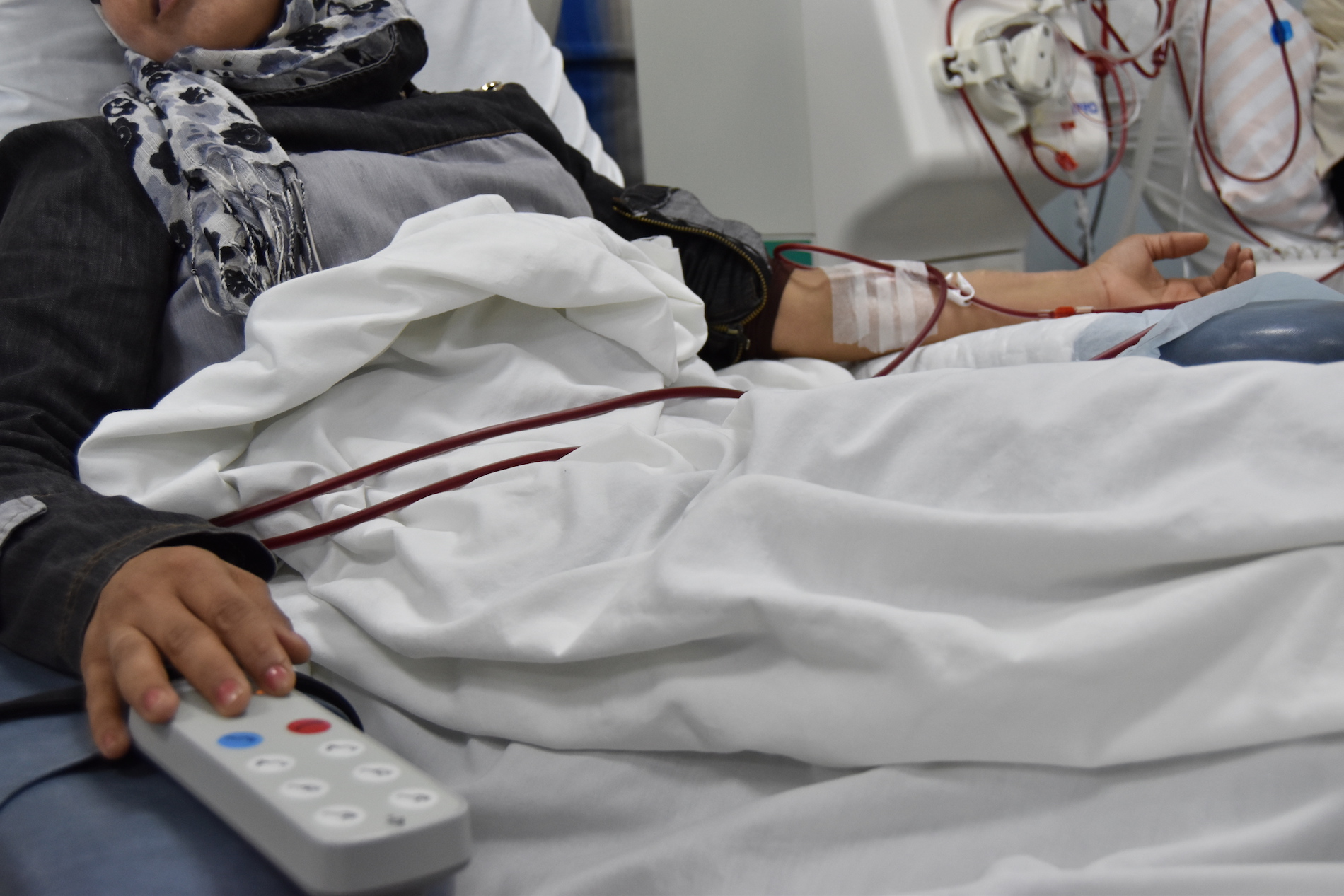
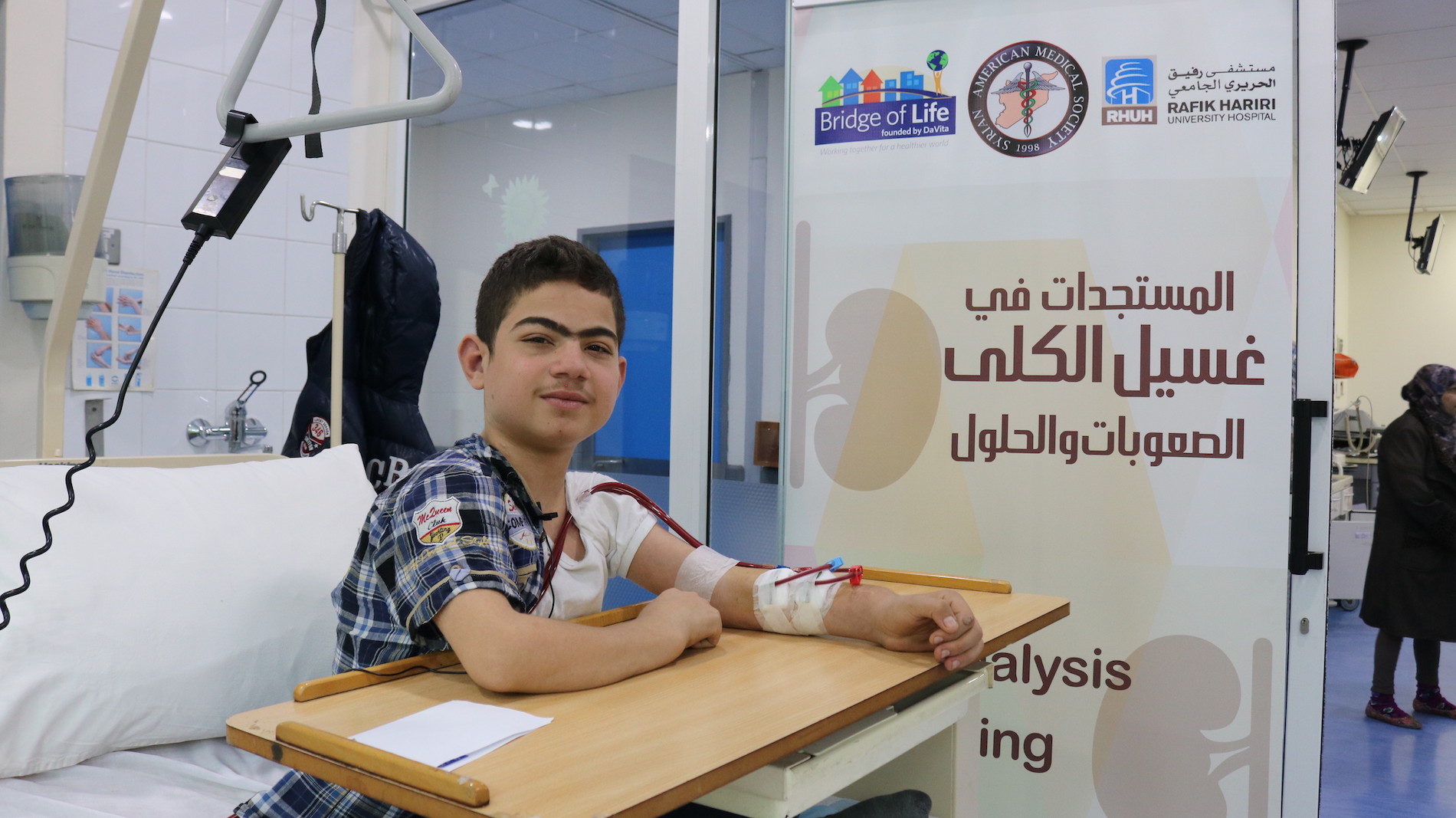
Haneen is a 12-year-old patient at a SAMS-supported dialysis center in Lebanon. Her journey started 6 months ago when high blood pressure led to the failure of one of her kidneys. While other youth her age are returning to school, Haneen must undergo dialysis treatment twice a week.
Haneen is a Syrian refugee living with her family in southern Lebanon in what can only be described as an inadequate and substandard shelter. Her father can occasionally find work, but not enough to cover basic food and shelter for the family, as well as treatment for Haneen. According to a vulnerability assessment by the United Nations, 76% of Syrian refugees in Lebanon live in extreme poverty, with food insecurity and poor access to basic needs, including health care.
Refugee communities in Lebanon face critical decisions every day, and Haneen’s father is no different as he struggles to balance costs of living against Haneen’s prohibitively expensive medical treatment. Refugees with renal failure need some of the most costly treatments in Lebanon, most requiring between 10 to 13 dialysis sessions per month in addition to medication. Each dialysis session costs a minimum of $110 and the medication runs, on average, over $300 a month. Many patients also need catheter treatment, which is not covered by UNHCR. UNHCR covers 75% to 90% of emergency and life-threatening services according to specific and restrictive criteria.
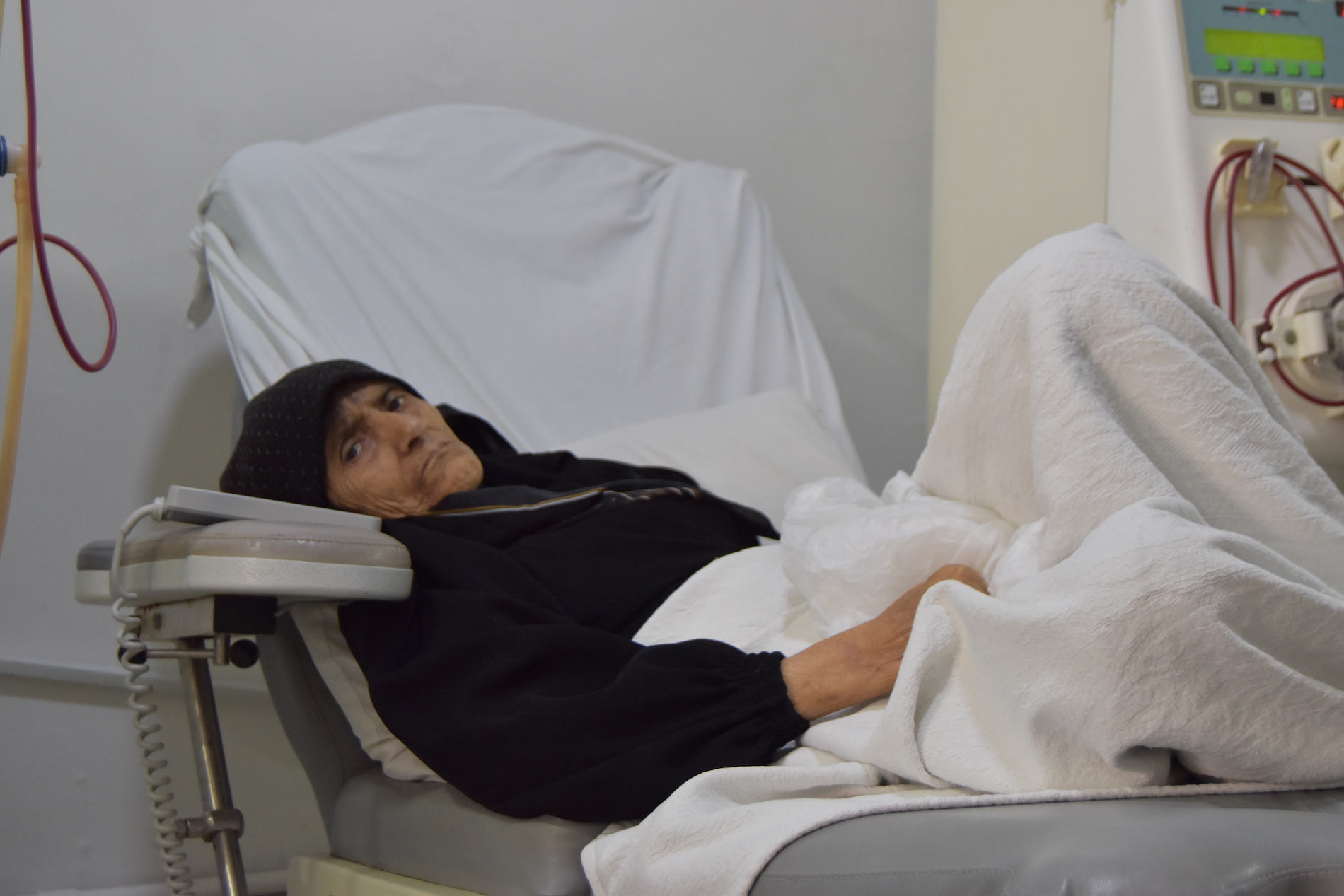
This gap leaves patients like Haneen particularly vulnerable. According to Lebanon’s Crisis Response Plan (2017-2020), approximately 200 registered refugees in Lebanon suffer from renal failure and require ongoing dialysis treatment. The plan is a key tool for the government of Lebanon, along with its international and national partners, and includes a multi-year plan to address the influx of refugees. While 110 of the patients identified with renal failure will receive one-year dialysis treatment according to the response plan, more than 60 patients remain on the waiting list. They have been unable to access treatment since early 2017. Despite immense efforts at the onset of the crisis to bolster the health sector in Lebanon, the public hospitals have accumulated a $15 million deficit and lack substantial national policies and strategies related to overcoming the health crisis.
This is the situation that Haneen faces.
“I waited for one month without treatment before SAMS was able to intervene. I had many complications [at first], and then I was enabled to live longer and better,” Haneen said.
Specialized services needed for patients with renal failure remain extremely limited and urgent. Only four major non-profit health organizations cover these cases- SAMS is one of them- and they are often unable to secure long-term funding. Despite calls for sufficient and sustainable funding to provide long-term services for dialysis patients, donors continue to focus on allocating funds for services that meet short-term needs.
SAMS works to fill this critical gap in dialysis care. SAMS has supported the treatment of 32 patients in need of hemodialysis in Lebanon since March 2017, providing treatment at two hospitals in Beka’a Valley, one in Beirut, and one in Tripoli. SAMS also organizes frequent medical missions to Lebanon that aim to follow up on patient cases and to evaluate the quality of services delivered in hospitals.
SAMS continues to advocate for appropriate funding for this incredibly vulnerable group, encouraging its own donors as well as advocating to other organizations in the humanitarian and medical fields. It has been difficult for SAMS to secure long-term funding for the dialysis patients most in need living in Syria’s neighboring countries.
The health sector in Lebanon suffers from a severe shortage of funding to support basic services for Syrian refugees, let alone specialized care. The percentage of funding in Lebanon showed a decrease in health coverage from 60% in August 2016 to 39% in 2018. Estimates suggest that it will take $290 million to provide healthcare for the nearly 1 million Syrian refugees in Lebanon in 2018. With only 39% covered, it is clear that the needs continue to outpace even current resources and capacities.
In addition to funding and prioritization challenges, structural obstacles pose another challenge that impedes patients with kidney failure from receiving treatment. Most facilities equipped to treat dialysis patients are located far from refugee settlements. In a survey conducted by the UNHCR, the majority of respondents mentioned they could not afford the transportation cost to access needed health services. Each time, Haneen travels to the hospital for her dialysis treatments and other check ups, the family pays more than $50. Many patients also lack legal documents and residence permits – meaning, they risk arrest, deportation, or other challenges as they travel to receive treatment.
The long term solution for patients like Haneen is a kidney transplant procedure. Haneen’s mother is a willing donor; however, the cost of the surgery is over $30,000. In the face of such a fee, many families turn to alternative methods to get by: borrowing money from friends and family, reducing essential food expenditures, and skipping dialysis sessions. Left with no other options, these coping mechanisms only serve to negatively impact the patient and their families.
The crisis in Syria has continued for more than half Haneen’s lifetime and has severely shortened her own life expectancy. Without long term sustainable treatment, Haneen and other dialysis patients can only wait each month and hope funding appears.
The impacts of war, violence, and civil strife are long lasting, and our commitment to their remedies should be equally sustained. Program implementation should be developed with plans that meet patient needs based on comprehensive studies of their physical, social, and economic situations. Donors must support the provision of public hospitals and primary health care clinics with specialty care services that are accessible to not only local communities, but refugees, IDPs, and other marginalized communities who are underserved.
This blog post was written by Ola Mouheildine, SAMS Advocacy Officer.